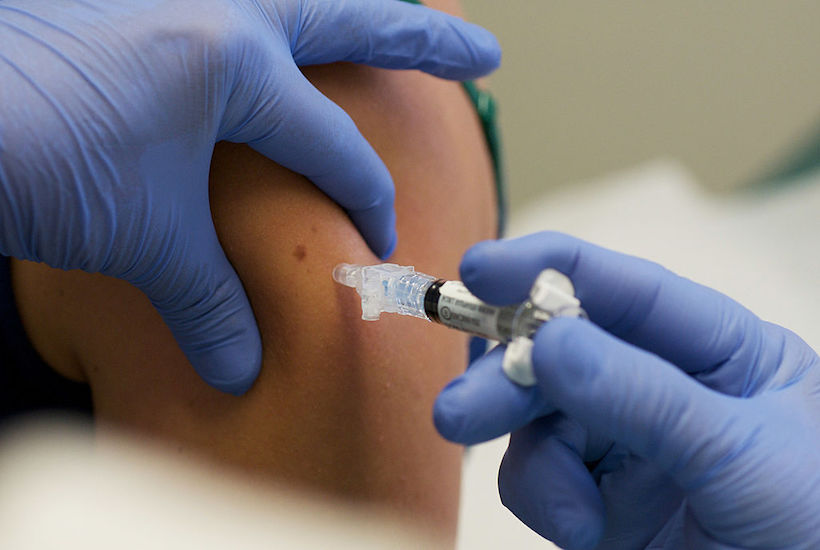
The COVID-19 pandemic has seen governments, universities and pharmaceutical companies in a mad scramble for a cure and a vaccine. That is a good and noble goal but we must be extremely careful to not cut corners in fast-tracking that noble goal. To do so would be nothing short of negligence on a grand scale.
Anti-vaxxers ignore decades of medical science and clinical trials, fearful of unfounded claims about harmful chemicals and side-effects like autism. However, there is a massive difference between being an anti-vaxxer and demanding a properly developed, tested and regulated vaccine — not to mention believing in individual liberty and basic bodily autonomy. Australia has agreed to purchase a vaccine currently being developed by Oxford University. That is a good proactive step, but Prime Minister Scott Morrison’s statement that he “would expect it to be as mandatory as you could possibly make it” needs clarification — especially when combined with the expectation that it could be ‘ready’ as early as next year (provided it ‘passes’ the current clinical trial stage).
People should have the right to take part in clinical trials, perhaps even encouraged to. I’m currently in one myself. There is an obvious reason why clinical trials are opt-in. Medicines can be dangerous and determining their benefits and side-effects is extremely uncertain but essential. Usually, clinical trials take a minimum of five years. While some of the process can be fast–tracked, the discovery of medium and long term side effects cannot be. To have a vaccine ‘pass’ a clinical trial in such a short time-frame is cause for alarm.
Even with well-established vaccines that have undergone clinical trials, there can be unforeseen issues. The 2010 bioCSL’s Fluvax influenza vaccine was associated with a higher rate of fever and fever-related convulsions in children under five than in previous influenza vaccines. It took a four-year investigation between CSL, the Australian regulator the Therapeutic Goods Administration and America’s Food and Drugs Administration to get to the likely cause of the increase; the relatively simple addition of new viral strains in that year’s vaccine.
All medicines are produced under Good Manufacturing Practices, GMP. Properly understanding and following GMP takes years of experience but its aims are simple; producing a product that is safe, effective and reliable. This cannot be rushed and therapeutic claims cannot rely on assumptions, wishful thinking and guesswork.
We have a great regulator in Australia (when they stick to their mandate) but they need realistic time-frames if they are to properly assess and evaluate the safety, efficacy and reliability of any vaccine. They cannot do that without sufficient data, which includes long and medium-term data on side-effects. Until that evaluation occurs to the usual standards that we expect, no vaccine should be publicly released and certainly not one with the expectation that it be “mandatory as you can possibly make it”.
The author is a medical scientist who works for one of Australia’s leading medical research organisations, has been in therapeutic quality management and regulatory affairs working with the TGA in conjunction with international regulators for over a decade and spoken on therapeutic quality management at Australian and international conferences. A pseudonym has been used to protect their privacy.