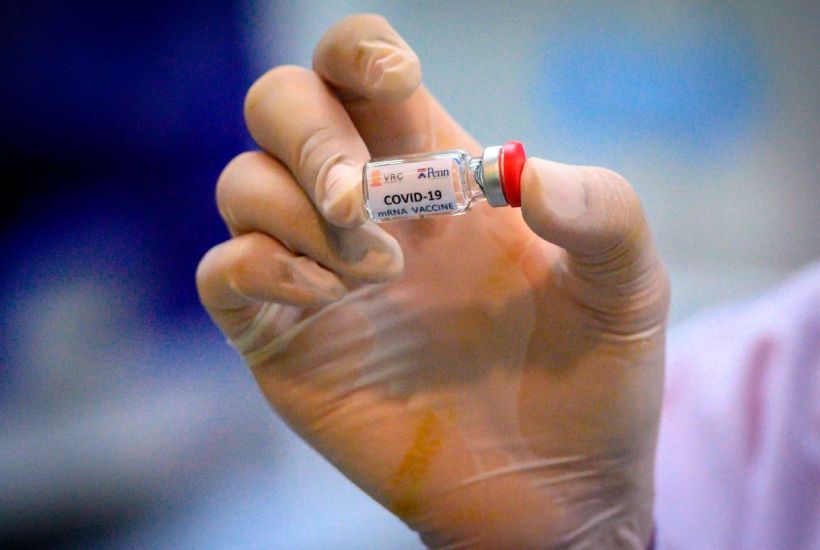
As billions wait with bated breath for the outcome of clinical trials on the new Covid-19 vaccines, many studies on other diseases have been halted. There are several reasons for this, not least the drop in revenue charities are receiving which is then used to fund studies. Additionally, coronavirus continues to dominate the medical landscape both in terms of the availability of doctors to do research and the willingness of patients to visit hospitals. Given the ongoing impact of the epidemic, it’s no surprise that so many resources are being piled into the search for a treatment for coronavirus. But this single-mindedness is coming at a great cost, not just for now but potentially for decades to come.
Clinical trial development of medical products such as drugs or equipment and devices are dependent on a lengthy and rigorous process. Because of a history of scandals, the process for approval of medicines for human use is now heavily regulated, expensive and time-consuming.
A candidate substance will start life in a small proof of concept trial (Phase 1) following experimental development with the main aim being overall safety. If all goes to plan, then a larger but still relatively small (Phase 2) study follows to try and measure if there is an appropriate treatment effect whilst gathering further safety information. Many seemingly promising drugs would have fallen by the wayside for various reasons by the time the next stage (Phase 3) has been reached. This is the last hurdle, which only a minority of prospective drugs attain. It is only after this stage that a company can apply for a license to drug regulatory authorities and start to market the medication.
The whole process can take up to ten years or more and costs many million pounds. I know first hand that the process of regulation and monitoring of safety is strict and there is also stringent post-marketing review which can remove a marketed drug from use if a new serious unexpected safety issue subsequently emerges. This is the ‘investment’ a pharmaceutical company, government or charity makes in funding this process. But the obvious prize is the development of a new, potentially life changing medicine – as well as riches for the successful company.
The other, and no less important, investment in this whole environment is made by those who permit themselves to be recruited to such trials. It often involves time off work, travel and increased medicalisation of their lives. There is also potential risk; we often do not fully know the safety of any new product.
Yet at a stroke, our response to coronavirus has hit the pause button on this long-established process of developing new medicines. Over 1,500 clinical trials have permanently closed and a further 9,000 have been suspended. Without these, medical science cannot advance and diseases will remain untreated. Patients will, ultimately, die as a result. And diseases which we might have found a cure for will remain untreatable.
As the NHS continues on its slow journey back to normality, the resumption of clinical trials must be viewed as a priority for our long-term health. It is likely with additional funding that a number of suspended trials can get on track again so that the net loss will be modest. But the future is also a concern. Recruitment to studies in the UK before the coronavirus epidemic was becoming increasingly challenging. Busy lives and difficulty fitting in trials into doctor’s schedules are just some of the reasons which has led to a shortfall of volunteers.
Whatever the future holds – and what 2020 has taught many is that planning ahead is not straightforward – we must prioritise clinical trials. Coronavirus still dominates the medical landscape, but other diseases have not stopped and neither should trials for new medicines