I have, in awe, seen a husband caring for his young wife—and their four children—in the last months of her life as she suffered from breast cancer. Then there is the woman who is currently looking after her physically healthy husband—of over fifty years—but is yet disintegrating mentally before her very eyes. These people are models of grace reflective of a greater power and love.
Contrastingly, in a grim sign of what is to come, Holland has now introduced legislation to euthanize patients suffering from dementia without their verbal consent! Words cannot adequately convey the horror and concern we should feel upon hearing of such a development.
Dr Hannah Graham (Lecturer in Criminology at the University of Sterling) and Dr Jeremy Prichard (Associate Professor at the University of Tasmania) have produced an excellent report which outlines the numerous reasons as to why legalising euthanasia is so problematic.
First, the bioethical. At the heart of this issue is the role of the medical professional. In particular, are they a healer, helper or killer? Significantly, a national survey in the United Kingdom has shown that the majority of doctors do not support the practice of euthanasia. What’s more, our own Australian Medical Association has also been highly critical of the practice. Dr Christopher Middleton has stated:
I think it would completely change the mind-set and the ethos of medicine in Australia because in their practice, in training, doctors tend to see themselves as agents of hope and healing and comfort, and certainly not as agents of death.
Second, the potential for elder abuse. The European Court of Human Rights has stated, “…that the risk of abuse inherent in a system which facilitated assisted suicide should not be underestimated.” As Dr Pritchard, in an op-ed for The Examiner writes:
In coming decades we face a rapidly aging population, a shrinking tax base and increases in health problems like dementia…euthanasia could form part of government planning for service provision for people nearing end-of-life…If that sounds far-fetched, consider two cases from Oregon where patients’ applications for medical treatment were rejected, but followed by departmental notifications informing the patients they were eligible for assisted dying.
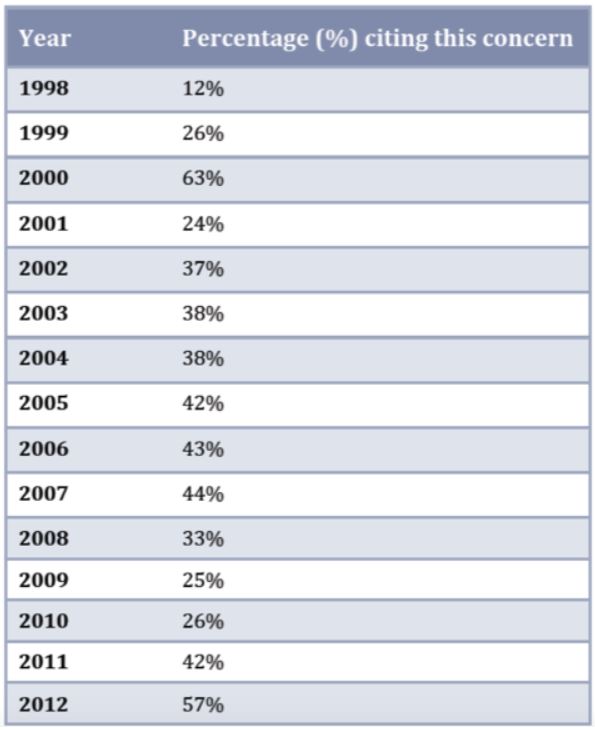
Third, the psychological pressure to end one’s life. Note the following table based on statistics from Oregon, which shows that since euthanasia has been made legal there has been a significant and steady increase in people giving the reason for choosing euthanasia so as not to be a burden on their family and friends.
 Fourth, is the negative societal perception of those who have a disability with their deaths being treated as an act of ‘compassion.’ Graham and Pritchard state that, “The implication that some people are ‘better off dead’ and that ‘some lives are not worth living’, phrases which have been used internationally in euthanasia debates, are potentially offensive and stigmatising to those who live with the same or similar symptoms and conditions.”
Fourth, is the negative societal perception of those who have a disability with their deaths being treated as an act of ‘compassion.’ Graham and Pritchard state that, “The implication that some people are ‘better off dead’ and that ‘some lives are not worth living’, phrases which have been used internationally in euthanasia debates, are potentially offensive and stigmatising to those who live with the same or similar symptoms and conditions.”
What’s more, euthanasia advocates, Loaran Bartels and Margaret Otlowski, argue that:
Since it is not unlawful for a person to commit or attempt to commit suicide, the law, implicitly at least, recognises the freedom of an individual to take her or his life. According to this argument, it follows that if an individual is free to commit suicide, he or she should arguably be able to seek the assistance of others in bringing this about.
However, as Constance Putnam has argued, there is a fundamental problem with framing the issue this way since “a ‘right to die’ is, in a very real sense, a curious concept. To have a ‘right’ to something that will inevitably take place regardless of circumstances or actions – like dying, for each of us – seems odd. I can think of no other right that any one of us might have to anything so universally (and absolutely predictably) inevitable.”
Fifth is “bracket creep.” What has been observed in countries that have legalised euthanasia is that the wishes of family members have pressured the patient to choose to be euthanised. What’s more, there is widespread under-reporting of the practice and there has also been a significant increase in the use of ‘terminal sedation’ resulting in the patient’s death. For instance, Dr Philip Nitschke, one of the leading proponents of legalising euthanasia, has been quoted as saying:
In the intervening 16 years since the Northern Territory Rights of the Terminally Ill Act came and went, the debate on voluntary euthanasia has been extended beyond those who are terminally ill, to include the well elderly (sic) for whom rational suicide is one of the many end of life options.
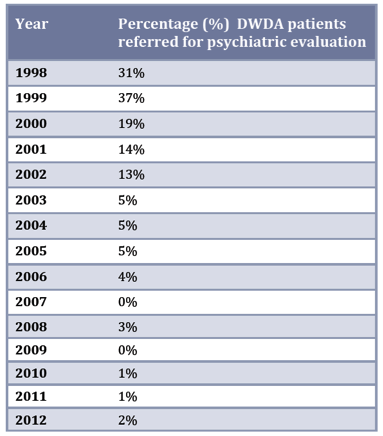
Sixth, the ‘safeguards’ of psychiatric referral and assessment are gradually ignored. Graham and Prichard state that, “In the Flanders region of Belgium approximately half of euthanasia cases are not formally monitored as doctors do not report them to authorities. The rate of underreporting in the Netherlands appears to be between 20-23 per cent.” What’s more, in Oregon, the percentage of people being referred for psychiatric evaluation has dramatically decreased, as can be seen in the following table:
 Seventh is the eventual practice and acceptance of non-voluntary euthanasia. In Belgium, where euthanasia has been legal since 2002, it has been observed that people were put to death without their consent. What’s more, nurses have taken upon themselves, without the presence of a doctor, the responsibility of administering euthanasia drugs.
Seventh is the eventual practice and acceptance of non-voluntary euthanasia. In Belgium, where euthanasia has been legal since 2002, it has been observed that people were put to death without their consent. What’s more, nurses have taken upon themselves, without the presence of a doctor, the responsibility of administering euthanasia drugs.
Eighth, numerous countries have examined and rejected it. No country should feel that they are on the “wrong side of history” in rejecting this practice when the majority of countries around the world have decided against its legalisation.
Ninth is the associated guilt that occurs when a medical professional is involved in ending another person’s life. For instance, Dr Kenneth Stevens, after researching this particular aspect, makes the following finding:
The physician is centrally involved in PAS and euthanasia, and the emotional and psychological effects on the participating physician can be substantial. The shift away from the fundamental values of medicine to heal and promote human wholeness can have significant effects on many participating physicians. Doctors describe being profoundly adversely affected, being shocked by the suddenness of the death, being caught up in the patient’s drive for assisted suicide, having a sense of powerlessness, and feeling isolated. There is evidence of pressure on and intimidation of doctors by some patients to assist in suicide. The effect of countertransference in the doctor-patient relationship may influence physician involvement in PAS and euthanasia.
Tenth, there are gendered risks, especially for women. There is a growing body of academic literature which highlights the ‘disproportionate victimisation of women’. As Prichard and Graham explain:
It is vitally necessary to carefully consider the potential for gendered violence and familial control to be directly or subtly influential, if not implicated, in matters of the ‘voluntary’ assisted death of women. Where there has been coercion, control and gendered violence in a woman’s life, the nature of which may often be kept hidden and secret from others (including in professional and personal relationships) in her life, it is important to ask whether this might be a factor in a woman’s death.
All of which is to say, the recent events that have taken place in Holland are a prescient warning as to some of the dangers that lie ahead in adopting it. Of course, they didn’t start out with that position when euthanasia was first legalised fifteen years ago, but it’s an example of what many people rightly fear will ultimately take place.
It makes you stop and ask yourself the question, “How would I like to be treated?” As a financial burden? A personal inconvenience? Or as those spouses I mentioned earlier acted towards their partners? With love. Compassion. And true dignity when I am most in need.
Mark Powell is the Associate Pastor of Cornerstone Presbyterian Church, Strathfield.
Got something to add? Join the discussion and comment below.